News and press releases
GRS seeks to provide clear and careful communication. Our demands on the comprehensibility and quality of information are based on the Guidelines for good science PR.

On 26 April 1986, the most serious nuclear accident since the beginning of the use of nuclear energy occurred at the Chernobyl nuclear power plant in Ukraine. Due to a series of operating errors and the special features of the reactor type, the power output rose sharply (causing the coolant to suddenly vaporise), the reactor core was completely destroyed and the graphite it contained caught fire. Around eight tonnes of radioactive fuel were released into the environment. To this day, there is an exclusion zone within a radius of 30 kilometres. The following article explains what happened on site during last year and how GRS supported the work there.

Last week, the Élysée Palace confirmed that the French reprocessing plant at La Hague is to be expanded. Extensive investments are planned in this context. There have already been plans since 2020 to build another storage pool on the plant site. At La Hague, there is still radioactive waste from Germany, which may be returned this year.

In Germany, around 1.1 million people live in so-called radon-prone areas. In these regions, a high radon concentration can be expected in significantly more buildings than the national average. The new GRS "Radon Dose" app estimates the personal radiation dose at the places of residence and work, based on measured or estimated radon levels.

The Russian invasion is affecting the lives and safety of people in Ukraine on many levels. With the capture of the nuclear power plant sites at Chernobyl - which is now back under Ukrainian control - and Zaporizhia, nuclear facilities have also been included in the hostilities and have therefore increasingly become the focus of public attention. GRS has been in close professional contact with Ukrainian partner organisations for decades, whereby the security of the facilties, i.e. their physical protection, also plays a role. On behalf of the Federal Foreign Office, GRS is working with Ukrainian and national partners to implement specific measures that contribute to improving the security of the facilities there.

Since the annexation of Crimea in 2014, GRS has been working with Ukrainian partners to strengthen the security of nuclear facilities in the country. The projects are funded by the German Federal Foreign Office (AA). In our interview, Dr Stephan Theimer, who heads one of these projects, talks about the challenges that the war poses for day-to-day work, what the current situation means for the security of the facilities, and what he would like to see in future cooperation.

What happened last year in the field of nuclear energy? What developments can be observed internationally? The following overview shows the situation broken down by continent (Europe, America, Asia and Africa). Australia/Oceania is not included, as no nuclear power plants are operated there. After a brief summary, those countries are presented for each continent which either operate reactors or which are planning to start or are already building NPPs.
The Office for Nuclear Regulation (ONR) published a statement yesterday (4 December 2023) after the Guardian newspaper reported cyberattacks on the Sellafield nuclear facility on the same day.

More than 30 pressurised water reactors of the Russian or Soviet VVER (water-water-energy reactor) type are currently in operation in Eastern and Central Europe, and several new plants are under construction. Mochovce-3, for example, started commercial operation in Slovakia in October 2023. Not least the war in Ukraine and the fact that the Zaporizhzhya nuclear power plant (NPP) became the theatre of war have shown that technical knowledge about this type of plant is still needed in Germany too, e.g. to be able to assess any risks. Experts at GRS are therefore involved in numerous research projects on VVER reactors, including international ones.
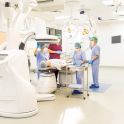
With the help of interventional radiology, certain medical procedures can be carried out in a minimally invasive manner that would previously have required surgery. As ionising radiation is generally used for imaging, the radiation exposure of the medical personnel involved has risen steadily over the years in line with the number of such procedures. In order to improve understanding of the distribution of radiation in the room and thus reduce radiation exposure, GRS scientists have produced a training video and a calculation tool as part of a research project funded by the German Federal Ministry for the Environment.

For many years there have been reports of radioactive caesium-137 (Cs-137) that is sometimes detected in large quantities in mushrooms and wild boar, especially in regions of southern Germany. Just in time for the start of the mushroom season, there have again been more reports of this in recent weeks. Where does the substance come from and why is it still detectable in larger quantities in mushrooms and wild boar, while it is decreasing overall in the ecosystem?